FEED ADVICE – HEALTH
Colic in Horse: Understanding and Prevention Tips
Colic in horses is a term used to describe abdominal pain rather than a specific diagnosis. It can stem from various gastrointestinal conditions as well as other causes of abdominal pain not related to the gastrointestinal tract.
Key Highlights

Colic in horses is defined as general abdominal pain and can encompass various different gastrointestinal conditions.
There are 6 defined types of colic which cover a broad spectrum of conditions.

Common clinical signs include rolling, pawing, frequent glancing at the flank and an increased heart rate.

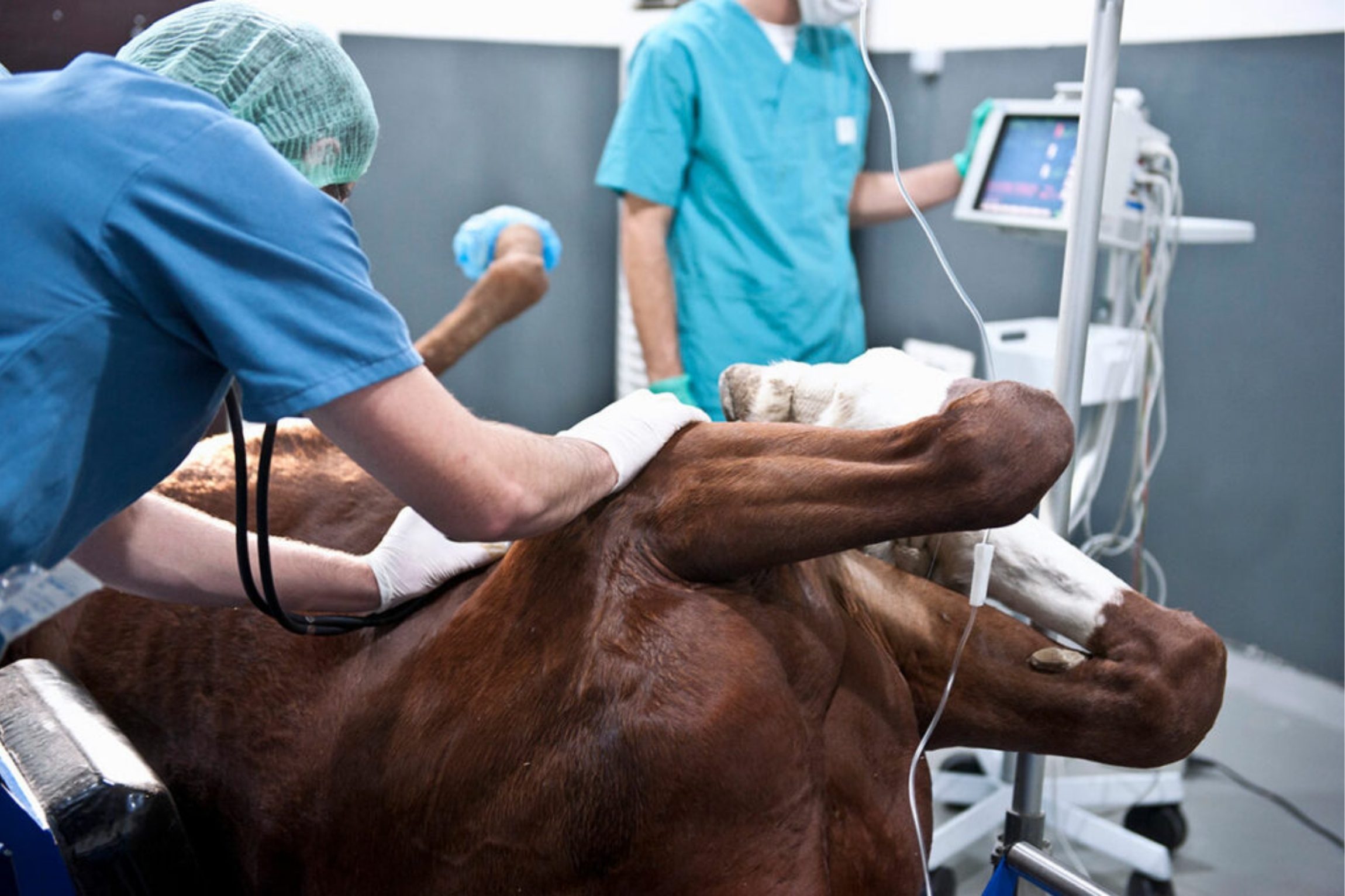
Rapid veterinary intervention is crucial, as colic can be fatal – early treatment can significantly improve the outcome and may prevent serious complications.
Understanding Colic
Colic in horses can stem from various causes, encompassing diet-related factors, stress, and environmental changes. Some of these factors include:
Dietary Factors: Rapid changes in type of feed or quantity, overconsumption of sugar, or feeding low-quality forage can disrupt the delicate balance of the digestive system, predisposing horses to colic.
Parasitic Infestation: Internal parasites, including tapeworms, pose a significant colic risk. Their presence can lead to inflammation, impaction, or obstruction of the intestines, contributing to colic episodes.
Grazing Management: Abrupt transitions from dry forage to lush pasture or inadequate turnout time can disrupt the horse’s digestive balance, leading to gastrointestinal upset and colic.
Stress and Environmental Factors: Horses are highly sensitive, and changes in routine, transportation, or confinement can induce stress, triggering colic symptoms. Additionally, environmental stressors such as extreme temperatures or social isolation can exacerbate the risk of colic.
Dental Health: Proper dental care is paramount for effective digestion in horses. Dental abnormalities, such as sharp points or malocclusions, can impede chewing and hinder the breakdown of feed particles, predisposing horses to colic.
Hydration Status: Inadequate water intake or dehydration can impair gastrointestinal motility, leading to impactions or sluggish bowel movements, common culprits of colic.

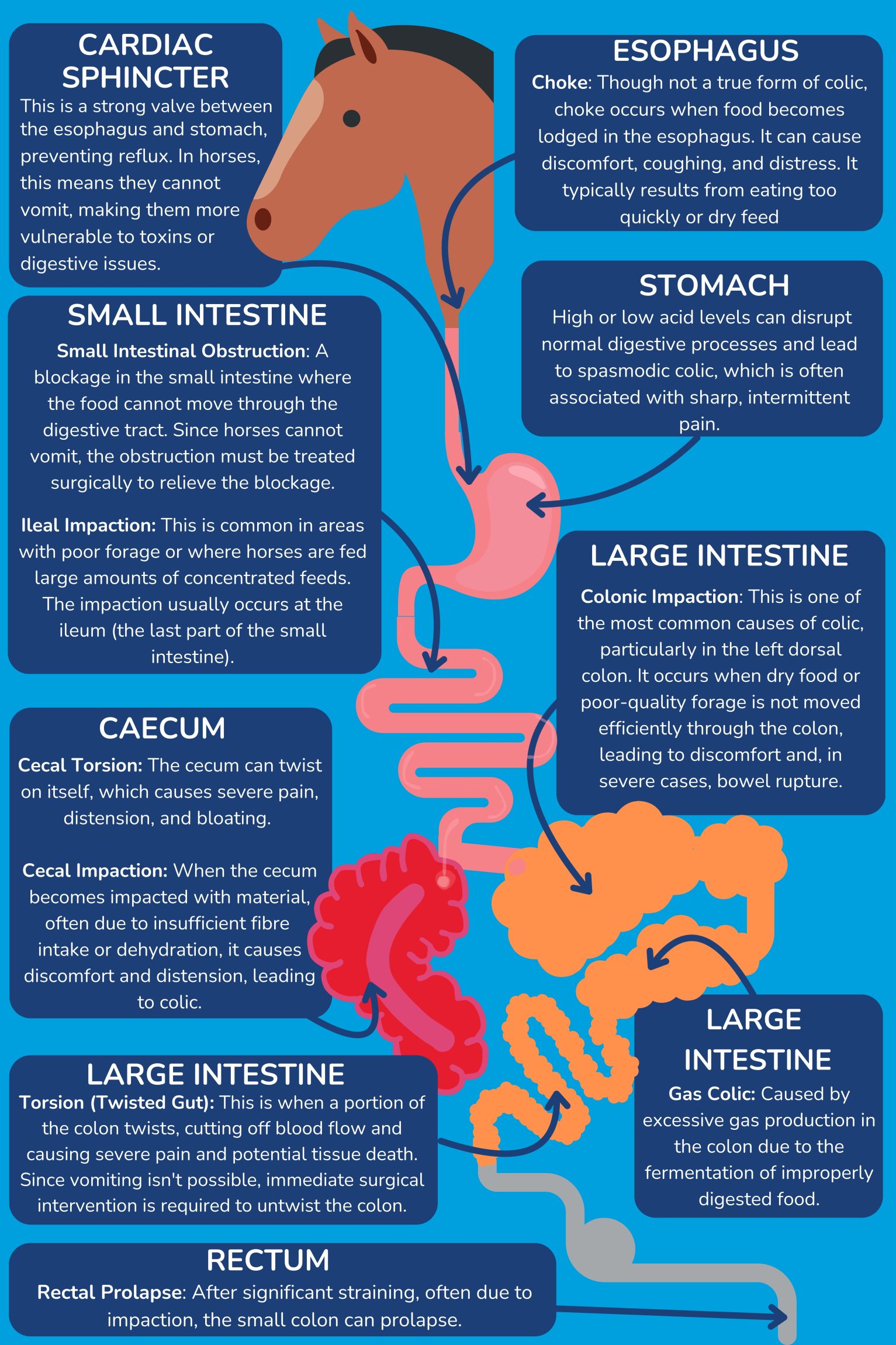
Types of Colic
There are 6 broad terms used to describe the different types of colic:
- Gas Colic: Characterised by the build-up of gas in the intestines, often due to fermentation of feed or sudden dietary changes. This accumulation causes distension and pain in the abdomen, typically manifesting as restlessness and discomfort in the affected horse.
- Impaction Colic: occurs when feed, sand, or other materials block the intestines, preventing normal passage. This blockage leads to severe abdominal pain, dehydration, and reduced appetite.
- Spasmodic Colic: caused by increased intestinal motility and muscle spasms, leading to intermittent and intense abdominal pain. It is often triggered by dietary changes, stress, or parasitic infections.
- Strangulation: occurs when the blood supply to a section of the intestine is cut off, often due to a twist or entrapment. This condition causes severe abdominal pain and rapid deterioration, necessitating emergency veterinary intervention and often surgery to prevent tissue death and further complications.
- Sand Colic: caused by the ingestion of sand or dirt, which accumulates in the horse’s intestines. This can lead to blockages, irritation, and inflammation, resulting in abdominal pain and discomfort.
- Displacement: occurs when a section of the intestine moves from its normal position, often causing a twist or blockage. This displacement can disrupt blood flow and digestion, leading to severe abdominal pain and requiring prompt veterinary intervention.
Recognising clinical signs of Colic
Behavioral changes and physical signs are crucial in recognising colic in horses.
Behavioural Changes:
Restlessness: The horse may appear anxious, pacing or unable to stand still.
Pawing: Repeatedly pawing at the ground is a common sign of discomfort.
Rolling: Horses with colic often roll to try and alleviate abdominal pain.
Sweating: Excessive sweating, particularly in the absence of exercise, is often a sign of distress.
Abdominal Stretching: The horse may stretch out as though trying to urinate, due to pain.
Lying Down and Standing Up: Repeatedly lying down and standing up can be a sign of discomfort and attempts to find relief.
Physical Changes:
Reduced or Absent Appetite: Horses with colic often refuse food or water due to pain.
Reduced or Absent Gut Sounds: A decrease or complete absence of gut sounds may indicate gut dysfunction.
Elevated Heart Rate: A heart rate above 48 beats per minute is a key indicator of colic-related distress.
Tachypnoea (Rapid Breathing): Breathing above 20 breaths per minute can signal pain or shock.
Temperature Changes: Normal body temperature ranges from 37.5°C to 38.5°C. A temperature drop below 37.0°C may indicate shock or severe colic.

Diagnosis of Colic
Diagnostic procedures for colic involve thorough examinations by vets. Early and accurate diagnosis is essential for providing the correct treatment swiftly.
1. Initial Examination Steps
During the initial examination of a colic horse, veterinarians focus on assessing vital signs such as heart rate and respiratory rate, as well as the hydration status and signs of abdominal pain.
- Heart Rate: An elevated heart rate (over 50 beats per minute) can indicate pain and stress. Severe colic often results in a heart rate exceeding 70 beats per minute.
- Respiratory Rate: An increased respiratory rate can accompany pain and stress.
- Mucous Membrane Colour: Checking the colour and moisture of the gums can provide clues about circulation and hydration. Pale or blue-tinged gums can indicate poor circulation or shock.
- Capillary Refill Time: Pressing on the gums and measuring the time it takes for colour to return helps assess blood flow and hydration status.
A rectal examination is often performed to assess the condition of the gastrointestinal tract. This involves a veterinarian manually examining the horse’s rectum. This can help identify specific types of colic, such as impaction, displacement, or twisted intestines.
2. Diagnostic Tools and Their Importance
Diagnostic tools play a crucial role in identifying the underlying causes of colic in horses. Technologies like ultrasound, endoscopy, and radiography aid veterinarians in assessing the severity and determining the most effective treatment plan. These tools provide detailed insights into the horse’s gastrointestinal tract, blood supply, and any abnormalities that may be contributing to the abdominal pain.
Nasogastric Intubation:
A tube is passed through the horse’s nose into the stomach to relieve built-up gas and fluid. The presence of reflux (large amounts of fluid) can indicate a blockage or severe motility issue in the intestines. This procedure also allows for the administration of medications directly into the stomach.
Ultrasound and Radiography:
Ultrasound: Non-invasive imaging to visualise the intestines, assess motility, and identify abnormalities such as displacements, blockages, or excessive fluid.
Radiography: X-rays can be particularly useful for diagnosing sand colic by showing the presence of sand or other foreign materials in the intestines.
Blood Tests:
Blood tests help evaluate the horse’s overall health and pinpoint specific issues.
Complete Blood Count (CBC): Assesses for signs of infection or inflammation.
Serum Chemistry: Evaluates organ function and electrolyte balance.
Lactate Levels: Elevated lactate levels can indicate poor blood flow to the intestines, a sign of severe or strangulating colic.
Prompt and accurate diagnosis is essential for effective treatment and can significantly impact the horse’s prognosis. Veterinary intervention should be sought at the first signs of colic to ensure the best possible outcome.


Treatment Options for Colic
The treatment for colic in horses depends on its severity and underlying cause. There are two main approaches: non-surgical management and surgical intervention.
Non-Surgical Management and Care
Non-surgical treatment focuses on pain relief, addressing dehydration, and managing the condition without surgery. The goal is to support the horse while avoiding invasive procedures when possible.
Fluid Therapy
Oral Fluids: Administered via a nasogastric tube to help rehydrate the horse and soften impactions.
Intravenous Fluids (IV): Used in severe cases to quickly correct dehydration and restore fluid balance.
Gastric Decompression
Repeated nasogastric intubation may be needed to relieve gas and fluid buildup in the stomach, particularly in cases of gas colic.
Controlled Walking
Helps stimulate intestinal motility and assists with the passage of gas or small impactions. However, excessive exercise should be avoided.
Dietary Management
Feed is temporarily withheld to allow the intestines to rest.
Small, easily digestible meals are gradually reintroduced as the horse shows improvement.
Medication Anti-Spasmodics: Drugs like Buscopan (hyoscine butylbromide) are used to relax intestinal spasms and relieve discomfort, particularly in cases of spasmodic colic.
Monitoring
Close observation of vital signs, such as heart rate, respiratory rate, and mucous membrane colour, is crucial to assess the horse’s response to treatment.
When Surgery Becomes a Necessity: What to Expect
If the horse does not improve with non-surgical management, or if it shows signs of severe distress, surgical intervention may be necessary. This could include:
Exploratory Abdominal Surgery: To investigate the cause of colic.
Intestinal Resection: Removing damaged sections of the intestine, if needed.
The primary surgical procedure is an exploratory laparotomy, where an incision is made into the abdomen to visually inspect the intestines. This allows veterinarians to identify the exact cause of colic, such as intestinal volvulus (twist), displacement, or strangulation. Depending on the findings, surgical corrections may include intestinal resection and anastomosis, where damaged portions of the intestine are removed and healthy ends reattached.
In cases of impaction, surgical decompression is necessary to relieve pressure and restore normal function. Surgical correction of intestinal strangulation is critical to untwist entrapped intestines and restore blood flow, preventing tissue death (necrosis) and further complications.
Post-surgical care involves intensive monitoring, pain management, fluid therapy, and careful reintroduction of food under veterinary supervision to ensure the horse’s recovery. Early detection and prompt surgical intervention significantly improve the chances of a successful outcome for horses suffering from colic.


Preventative Measures Against Colic
Implementing preventative measures is crucial for preventing colic episodes. Key strategies include maintaining a consistent and balanced diet to prevent digestive issues. Avoid sudden dietary changes and ensure access to clean cold water. Regular exercise can also aid in promoting healthy gut function. Routine veterinary check-ups and proper dental care are essential. Additionally, controlling environmental factors such as stress and ensuring a suitable living environment can minimize the risk of colic.
Dietary Management and Feeding Practices
Implementing proper dietary management and feeding practices is crucial in preventing colic in horses. Key strategies include:
- Balanced Diets: Providing horses with well-balanced diets rich in high-quality forage, essential nutrients, and adequate fibre content promotes optimal gastrointestinal health and reduces the risk of digestive disturbances.
- Gradual Diet Transitions: Abrupt changes in feed composition or quantity should be avoided, as they can disrupt the delicate microbial ecosystem within the gut and predispose horses to colic – did you know that all Pure Feed’s complete feeds share the same core ingredients? This means you can switch between all of the complete feeds with no transition time without risking colic!
- Forage Management: Regular access to clean, quality forage supports proper digestion, maintains gut motility, and minimizes the risk of impaction colic.
- Supplements: using probiotics, prebiotics, and digestive enzymes can support gastrointestinal health, enhance nutrient absorption, and fortify the gut barrier function – did you know all of our complete feeds already contain pre and probiotics to make sure your horse’s digestive system is supported!
- Hydration Maintenance: Adequate water intake is essential for optimal digestive function and overall well-being. Monitoring water availability and quality ensures horses remain adequately hydrated, mitigating the risk of colic associated with dehydration – Check out our Meadow Mash or ReFuel if your horse needs help drinking!
Routine Health Care and Monitoring
Regular and routine healthcare and monitoring are essential components of effective horse management to prevent and promptly detect colic. Establishing and adhering to a consistent healthcare regimen, which includes regular dental check-ups, deworming schedules, and vaccinations, is crucial. Monitoring vital signs such as temperature, heart rate, and gut sounds on a regular basis facilitates early detection of colic. It’s important to be familiar with your horse’s baseline values to accurately assess any deviations.
Conclusion
In summary, colic poses a serious health risk to horses, demanding proactive care and attentive management from owners. Swift recognition of symptoms, immediate veterinary attention, and consistent preventive measures are crucial for preventing colic episodes. By being consistent with healthcare routines such as worming, ensuring balanced nutrition, and closely monitoring behaviour and vital signs, owners can effectively reduce the likelihood and severity of colic episodes, promoting the long-term health and happiness of their horses.
Featured products for horses prone to colic
Made in the UK
We are proud to say that all of our feeds are produced here in the UK
FREE Shipping
We offer FREE SHIPPING for all orders in the UK with 15 bags and over*
Sustainable
We are dedicated to playing our part in making the world more sustainable

100% Natural
We use high-quality ingredients and no unnecessary additives.
Thousands of people love our feeds
It’s finally here!! Badminton week! We’re wishing our brand ambassador @ellah.orses the biggest luck and can’t wait to cheer her down the centreline at 14:36 today! 🍀🩵

It’s finally here!! Badminton week! We’re wishing our brand ambassador @ellah.orses the biggest luck and can’t wait to cheer her down the centreline at 14:36 today! 🍀🩵
May just got better 🌱
£5 off Pure Stud, all month long!
Complete nutrition for youngstock, mares & stallions… without the extras you don’t want.
✔ No cereals
✔ No molasses
✔ No soya or alfalfa
✔ Low sugar & starch
Available in-store & online 🩵

May just got better 🌱
£5 off Pure Stud, all month long!
Complete nutrition for youngstock, mares & stallions… without the extras you don’t want.
✔ No cereals
✔ No molasses
✔ No soya or alfalfa
✔ Low sugar & starch
Available in-store & online 🩵
Did you know the sugar in grass isn’t constant?
It rises and falls throughout the day, driven by photosynthesis and temperature. Early morning (6–10 am), photosynthesis hasn’t yet packed the grass with soluble sugars, so grazing is generally lower risk and a safer window for horses prone to laminitis or weight gain.
Between late morning and late afternoon (11–5 pm), sunlight drives sugar production. Levels climb steadily, meaning horses grazing during this period should be monitored closely, especially those with metabolic sensitivities.
By evening and overnight (18–05 am), grass sugar can peak. Cooler nights trap sugars in the plant, creating a riskier forage for susceptible horses. Grazing unmanaged during this window can overload the horse’s system and trigger laminitis.
Understanding these daily sugar fluctuations allows you to manage turnout strategically, protect gut and metabolic health.

Did you know the sugar in grass isn’t constant?
It rises and falls throughout the day, driven by photosynthesis and temperature. Early morning (6–10 am), photosynthesis hasn’t yet packed the grass with soluble sugars, so grazing is generally lower risk and a safer window for horses prone to laminitis or weight gain.
Between late morning and late afternoon (11–5 pm), sunlight drives sugar production. Levels climb steadily, meaning horses grazing during this period should be monitored closely, especially those with metabolic sensitivities.
By evening and overnight (18–05 am), grass sugar can peak. Cooler nights trap sugars in the plant, creating a riskier forage for susceptible horses. Grazing unmanaged during this window can overload the horse’s system and trigger laminitis.
Understanding these daily sugar fluctuations allows you to manage turnout strategically, protect gut and metabolic health.
Growth places specific nutritional demands on young horses, requiring a precise balance of energy, protein, vitamins and minerals to support correct development.
Pure Stud is formulated to deliver this in a controlled way; high in fibre to support the digestive system, low in sugar and starch to avoid unnecessary peaks in blood glucose and insulin, and with a built-in stud balancer to provide essential vitamins, minerals and quality amino acids.
This supports steady growth rates, skeletal development, and muscle formation without relying on high-starch, high-calorie formulations.
A consistent, balanced approach to nutrition during growth is key to supporting long-term soundness and development.

Growth places specific nutritional demands on young horses, requiring a precise balance of energy, protein, vitamins and minerals to support correct development.
Pure Stud is formulated to deliver this in a controlled way; high in fibre to support the digestive system, low in sugar and starch to avoid unnecessary peaks in blood glucose and insulin, and with a built-in stud balancer to provide essential vitamins, minerals and quality amino acids.
This supports steady growth rates, skeletal development, and muscle formation without relying on high-starch, high-calorie formulations.
A consistent, balanced approach to nutrition during growth is key to supporting long-term soundness and development.
One bag. No gaps. No guesswork.
Feeding shouldn’t feel like a balancing act. That’s why our feeds are built differently - truly complete, with everything your horse needs in every single mouthful:
🌱 Multiple fibre sources (grass pellets + chaff) for gut health and chew time
⚡ Slow-release energy from linseed, rapeseed oil & unmolassed sugar beet
🧬 A fully balanced vitamin & mineral package
💪 Essential amino acids for muscle support
🦶 Biotin for strong hooves
🧂 Salt for hydration and electrolyte balance
🦠 Pre & probiotics for optimal digestion
No extras. No add-ons. Just Pure Feed 🩵

One bag. No gaps. No guesswork.
Feeding shouldn’t feel like a balancing act. That’s why our feeds are built differently - truly complete, with everything your horse needs in every single mouthful:
🌱 Multiple fibre sources (grass pellets + chaff) for gut health and chew time
⚡ Slow-release energy from linseed, rapeseed oil & unmolassed sugar beet
🧬 A fully balanced vitamin & mineral package
💪 Essential amino acids for muscle support
🦶 Biotin for strong hooves
🧂 Salt for hydration and electrolyte balance
🦠 Pre & probiotics for optimal digestion
No extras. No add-ons. Just Pure Feed 🩵
If you’ve ever owned a good-doer, you’ll know… they don’t miss a meal. Not ever.
Spring grass comes through, the sun appears, and suddenly, what should be a simple turnout becomes a stressful balancing act.
For some, that starts with a muzzle. Not to restrict completely, but to slow things down – turning every bite into a more considered mouthful.
For others, it’s strip grazing. Walking the fence line forward inch by inch, controlling access to fresh grass and keeping intake steady rather than excessive.
Then there’s hay, soaked to reduce sugar levels, making it a safer, more suitable forage option when you need to take the edge off.
Some horses thrive in dry paddocks, where grass intake is minimal but movement and turnout are still part of their routine. Others benefit from a little more time stabled, where you can fully manage what goes in and when.
All of these approaches share the same underlying principle: restriction. You’re limiting intake to manage weight, sugar exposure, and overall health. But it’s easy to forget what else gets restricted at the same time. When you reduce grass, soak hay, or limit access to forage, you’re not just cutting calories and sugars, you’re also reducing the intake of essential vitamins, minerals, and amino acids that your horse would naturally pick up throughout the day.
Over time, that gap can start to show. Hoof quality, coat condition, muscle maintenance, even energy levels and recovery, they’re all influenced by those nutrients that are no longer consistently coming in. This is where a low calorie balancer, like Pure Balance comes in. It`s job is to fill in these nutrition gaps and help provide your horse with everything they need, in a low calorie format 🩵

If you’ve ever owned a good-doer, you’ll know… they don’t miss a meal. Not ever.
Spring grass comes through, the sun appears, and suddenly, what should be a simple turnout becomes a stressful balancing act.
For some, that starts with a muzzle. Not to restrict completely, but to slow things down – turning every bite into a more considered mouthful.
For others, it’s strip grazing. Walking the fence line forward inch by inch, controlling access to fresh grass and keeping intake steady rather than excessive.
Then there’s hay, soaked to reduce sugar levels, making it a safer, more suitable forage option when you need to take the edge off.
Some horses thrive in dry paddocks, where grass intake is minimal but movement and turnout are still part of their routine. Others benefit from a little more time stabled, where you can fully manage what goes in and when.
All of these approaches share the same underlying principle: restriction. You’re limiting intake to manage weight, sugar exposure, and overall health. But it’s easy to forget what else gets restricted at the same time. When you reduce grass, soak hay, or limit access to forage, you’re not just cutting calories and sugars, you’re also reducing the intake of essential vitamins, minerals, and amino acids that your horse would naturally pick up throughout the day.
Over time, that gap can start to show. Hoof quality, coat condition, muscle maintenance, even energy levels and recovery, they’re all influenced by those nutrients that are no longer consistently coming in. This is where a low calorie balancer, like Pure Balance comes in. It`s job is to fill in these nutrition gaps and help provide your horse with everything they need, in a low calorie format 🩵
✨ Pure Fibre Balance - high-fibre, low-calorie feed for good doers! ✨
Combines our premium balancer pellets (vitamins, minerals, pre/probiotics, biotin, amino acids, salt) with low-calorie chaff for extra fibre to provide steady, slow-release energy (no fizz) = ideal for good doers & laminitis-prone horses
🚫 Cereal & molasses free, no preservatives – all the nutrition, none of the empty calories 🩵

✨ Pure Fibre Balance - high-fibre, low-calorie feed for good doers! ✨
Combines our premium balancer pellets (vitamins, minerals, pre/probiotics, biotin, amino acids, salt) with low-calorie chaff for extra fibre to provide steady, slow-release energy (no fizz) = ideal for good doers & laminitis-prone horses
🚫 Cereal & molasses free, no preservatives – all the nutrition, none of the empty calories 🩵
A good session doesn’t end when you untack.
Work takes more out of your horse than you can always see: fluid loss through sweat, muscles under strain, and a digestive system that’s more sensitive post-exercise.
That’s where Refuel comes in.
Supporting faster muscle recovery, replenishing electrolytes for effective hydration, and formulated to be gut safe, it helps your horse recover properly 🩵

A good session doesn’t end when you untack.
Work takes more out of your horse than you can always see: fluid loss through sweat, muscles under strain, and a digestive system that’s more sensitive post-exercise.
That’s where Refuel comes in.
Supporting faster muscle recovery, replenishing electrolytes for effective hydration, and formulated to be gut safe, it helps your horse recover properly 🩵
Both Fibre Balance and Easy are part of our low calorie range but which suits your horse?
Pure Fibre Balance is built for good-doers who don’t need extra energy - low calorie, high fibre, fully balanced, and ideal for those in light work or at maintenance. It is like feeding a full cup of balancer with a handful of chaff. Everything your horse needs in one measured portion: high fibre, low sugar and starch, perfectly balanced.
Pure Easy uses the same ingredients, but served at a higher rate – more fibre, more slow-release energy, without adding extra sugar or starch. It’s the choice for horses that need extra bulk and sustained energy, while staying completely balanced and gut-friendly.
Not sure which would be best for your horse? Comment `DIET PLAN` to recieve a link to our diet plan 🩵

Both Fibre Balance and Easy are part of our low calorie range but which suits your horse?
Pure Fibre Balance is built for good-doers who don’t need extra energy - low calorie, high fibre, fully balanced, and ideal for those in light work or at maintenance. It is like feeding a full cup of balancer with a handful of chaff. Everything your horse needs in one measured portion: high fibre, low sugar and starch, perfectly balanced.
Pure Easy uses the same ingredients, but served at a higher rate – more fibre, more slow-release energy, without adding extra sugar or starch. It’s the choice for horses that need extra bulk and sustained energy, while staying completely balanced and gut-friendly.
Not sure which would be best for your horse? Comment `DIET PLAN` to recieve a link to our diet plan 🩵
Different workloads, different grazing, different quirks that make “one size fits all” feeding… not quite fit at all. That’s usually where the questions start.
"Am I feeding too much? Not enough? The right balance?"
Our diet plan service takes the guesswork out of it. A quick, simple form, reviewed by our nutritionists, and within a day, you’ve got a plan built specifically for your horse – their needs, their lifestyle, their routine.
👉 Comment `DIET PLAN` to find out more 🩵

Different workloads, different grazing, different quirks that make “one size fits all” feeding… not quite fit at all. That’s usually where the questions start.
"Am I feeding too much? Not enough? The right balance?"
Our diet plan service takes the guesswork out of it. A quick, simple form, reviewed by our nutritionists, and within a day, you’ve got a plan built specifically for your horse – their needs, their lifestyle, their routine.
👉 Comment `DIET PLAN` to find out more 🩵
Keep your good doers in top condition without overloading them with calories! 🌿🐴
Pure Easy is a low-calorie, low sugar and starch feed designed specifically for horses that gain weight easily. Despite the lower calories, it provides steady, slow-release energy from high-quality fibre and superfibre sources, perfect for horses in light to medium work.
It also contains a built-in balancer packed with essential vitamins, minerals, pre- & probiotics to support the gut microbiome, biotin for strong hooves, key amino acids for muscle maintenance, and added salt to help hydration.
This carefully formulated feed lets you give your horse the energy they need to perform, without risking excess weight gain , all in one simple, easy feed! 🩵

Keep your good doers in top condition without overloading them with calories! 🌿🐴
Pure Easy is a low-calorie, low sugar and starch feed designed specifically for horses that gain weight easily. Despite the lower calories, it provides steady, slow-release energy from high-quality fibre and superfibre sources, perfect for horses in light to medium work.
It also contains a built-in balancer packed with essential vitamins, minerals, pre- & probiotics to support the gut microbiome, biotin for strong hooves, key amino acids for muscle maintenance, and added salt to help hydration.
This carefully formulated feed lets you give your horse the energy they need to perform, without risking excess weight gain , all in one simple, easy feed! 🩵
Did you know Vitamin E, or Tocopheryl, is crucial for your horse’s overall health? All Pure Complete feeds include it in our balancer, ensuring your horse gets the benefits every day:
👉 Protects cells from oxidative stress – helping to neutralise free radicals.
👉 Supports muscle function and recovery – essential for exercise and stamina.
👉 Maintains a normal immune system – keeping your horse strong and resilient.
Including Vitamin E in every feed means your horse receives targeted antioxidant support alongside all the vitamins, minerals, and nutrients in our balancer. Perfect for keeping horses happy and performing at their best! 🌿

Did you know Vitamin E, or Tocopheryl, is crucial for your horse’s overall health? All Pure Complete feeds include it in our balancer, ensuring your horse gets the benefits every day:
👉 Protects cells from oxidative stress – helping to neutralise free radicals.
👉 Supports muscle function and recovery – essential for exercise and stamina.
👉 Maintains a normal immune system – keeping your horse strong and resilient.
Including Vitamin E in every feed means your horse receives targeted antioxidant support alongside all the vitamins, minerals, and nutrients in our balancer. Perfect for keeping horses happy and performing at their best! 🌿
Refuel comes with a splash zone warning!
A recovery mash horses just can`t get enough of! Packed with electrolytes, antioxidants and amino acids, Refuel works hard to keep your horse in tip top shape!
We would love to see a photo of your horse after a bowl of Refuel, drop them in the comments below 👇

Refuel comes with a splash zone warning!
A recovery mash horses just can`t get enough of! Packed with electrolytes, antioxidants and amino acids, Refuel works hard to keep your horse in tip top shape!
We would love to see a photo of your horse after a bowl of Refuel, drop them in the comments below 👇
Body condition scoring… we talk about it a lot, but what does it actually look like in practice? 👀
It’s not about one quick glance or a number on a chart, it’s about building a picture, piece by piece, of how your horse is carrying condition.
1. Start at the topline.
Run your hand along the back: are the vertebrae sharp and visible, or is there a smooth, even covering? Ideally, you’re looking for a soft, rounded feel without a crease forming down the spine, which can indicate excess fat.
2.Then move to the neck and shoulders.
This is where fat can start to deposit quite early. A cresty neck or filling in front of the shoulder can be a sign your horse is carrying more condition than they need, particularly in native types or good doers. It’s also an important area to monitor for metabolic health.
3. Next, the ribs.
You shouldn’t necessarily see them, but you should be able to feel them easily. If they’re hard to find, it’s often a sign condition is creeping up. If they’re too prominent, it may indicate your horse needs more support nutritionally.
4. Then the hindquarters.
Look at the shape; are they rounded and filled, or more angular? Fat tends to sit around the tail head and quarters, so this area gives a good indication of overall energy balance.
And finally and most importantly, monitor over time.
Body condition scoring isn’t a one-off check. Horses change with the seasons, workload, and diet. What matters is spotting those small changes early, before they become bigger issues. Because when you understand where and how your horse carries condition, you’re in a much better position to feed for them, not just follow a generic plan.
Not sure what you’re feeling for? We’re always happy to help 👇

Body condition scoring… we talk about it a lot, but what does it actually look like in practice? 👀
It’s not about one quick glance or a number on a chart, it’s about building a picture, piece by piece, of how your horse is carrying condition.
1. Start at the topline.
Run your hand along the back: are the vertebrae sharp and visible, or is there a smooth, even covering? Ideally, you’re looking for a soft, rounded feel without a crease forming down the spine, which can indicate excess fat.
2.Then move to the neck and shoulders.
This is where fat can start to deposit quite early. A cresty neck or filling in front of the shoulder can be a sign your horse is carrying more condition than they need, particularly in native types or good doers. It’s also an important area to monitor for metabolic health.
3. Next, the ribs.
You shouldn’t necessarily see them, but you should be able to feel them easily. If they’re hard to find, it’s often a sign condition is creeping up. If they’re too prominent, it may indicate your horse needs more support nutritionally.
4. Then the hindquarters.
Look at the shape; are they rounded and filled, or more angular? Fat tends to sit around the tail head and quarters, so this area gives a good indication of overall energy balance.
And finally and most importantly, monitor over time.
Body condition scoring isn’t a one-off check. Horses change with the seasons, workload, and diet. What matters is spotting those small changes early, before they become bigger issues. Because when you understand where and how your horse carries condition, you’re in a much better position to feed for them, not just follow a generic plan.
Not sure what you’re feeling for? We’re always happy to help 👇
In the UK, it’s estimated that 1 in 10 horses will experience a laminitis episode every year; that’s around 96,000 cases annually.
And right now, in April, we’re entering one of the highest-risk periods of the year.
As grass growth accelerates with longer days and fluctuating temperatures, levels of non-structural carbohydrates (NSCs), particularly sugars like fructans, can rise significantly. Cool nights followed by bright, sunny days are the perfect conditions for these sugar levels to spike, increasing the risk for horses, especially those with underlying insulin dysregulation.
Laminitis is now widely recognised as a complex, endocrine-driven disease, where elevated insulin levels can directly compromise the lamellar structures within the hoof. This weakens the bond between the hoof wall and pedal bone, and once damage begins, it can progress quickly, leading to chronic pain, mechanical failure, and in severe cases, irreversible collapse.
It’s for this reason that laminitis remains one of the leading causes of death in horses in the UK, with many cases ending in euthanasia on welfare grounds.
From a nutritional perspective, prevention at this time of year is critical. It’s not just about restricting grazing, but about taking a proactive, whole-diet approach:
• Managing total NSC intake across forage and feed
• Supporting hindgut function and fibre digestion
• Avoiding sudden dietary changes
• Maintaining a normal body condition and metabolic balance
At Pure Feed, we’re proud that our feeds are formulated to be suitable for horses with laminitis; carefully designed to be low in sugar and starch, high in fibre, and supportive of normal metabolic function, helping you manage risk without compromising on nutrition.
If you’re unsure whether your horse’s diet is appropriate for this time of year, our team is always here to help; comment below, DM us or give our team a call on 01458 333333 🩵

In the UK, it’s estimated that 1 in 10 horses will experience a laminitis episode every year; that’s around 96,000 cases annually.
And right now, in April, we’re entering one of the highest-risk periods of the year.
As grass growth accelerates with longer days and fluctuating temperatures, levels of non-structural carbohydrates (NSCs), particularly sugars like fructans, can rise significantly. Cool nights followed by bright, sunny days are the perfect conditions for these sugar levels to spike, increasing the risk for horses, especially those with underlying insulin dysregulation.
Laminitis is now widely recognised as a complex, endocrine-driven disease, where elevated insulin levels can directly compromise the lamellar structures within the hoof. This weakens the bond between the hoof wall and pedal bone, and once damage begins, it can progress quickly, leading to chronic pain, mechanical failure, and in severe cases, irreversible collapse.
It’s for this reason that laminitis remains one of the leading causes of death in horses in the UK, with many cases ending in euthanasia on welfare grounds.
From a nutritional perspective, prevention at this time of year is critical. It’s not just about restricting grazing, but about taking a proactive, whole-diet approach:
• Managing total NSC intake across forage and feed
• Supporting hindgut function and fibre digestion
• Avoiding sudden dietary changes
• Maintaining a normal body condition and metabolic balance
At Pure Feed, we’re proud that our feeds are formulated to be suitable for horses with laminitis; carefully designed to be low in sugar and starch, high in fibre, and supportive of normal metabolic function, helping you manage risk without compromising on nutrition.
If you’re unsure whether your horse’s diet is appropriate for this time of year, our team is always here to help; comment below, DM us or give our team a call on 01458 333333 🩵
Did you know we use linseed in all of our feeds? Linseed is a powerhouse ingredient that brings multiple benefits to every feed. Here’s why we use it in all Pure Feed products:
1️⃣ Natural binder: Linseed contains mucilage, a sticky soluble fibre that binds feed pellets together naturally. This eliminates the need for molasses, so we can produce stable, consistent pellets without added sugar. For horses, this means better metabolic health and reduced risk of sugar-related issues.
2️⃣ Rich in Omega-3 fatty acids: Linseed provides essential fatty acids that support skin, coat, joint, and heart health, while also helping to maintain a normal inflammatory balance.
3️⃣ Gut-friendly fibre: The soluble fibre in linseed acts as a prebiotic, supporting beneficial gut microbes and improving nutrient absorption.
By using linseed instead of molasses, we combine function, nutrition, and safety, creating a feed that’s not only easier to handle and more palatable but also better for your horse’s long-term wellbeing!

Did you know we use linseed in all of our feeds? Linseed is a powerhouse ingredient that brings multiple benefits to every feed. Here’s why we use it in all Pure Feed products:
1️⃣ Natural binder: Linseed contains mucilage, a sticky soluble fibre that binds feed pellets together naturally. This eliminates the need for molasses, so we can produce stable, consistent pellets without added sugar. For horses, this means better metabolic health and reduced risk of sugar-related issues.
2️⃣ Rich in Omega-3 fatty acids: Linseed provides essential fatty acids that support skin, coat, joint, and heart health, while also helping to maintain a normal inflammatory balance.
3️⃣ Gut-friendly fibre: The soluble fibre in linseed acts as a prebiotic, supporting beneficial gut microbes and improving nutrient absorption.
By using linseed instead of molasses, we combine function, nutrition, and safety, creating a feed that’s not only easier to handle and more palatable but also better for your horse’s long-term wellbeing!
Feeding shouldn’t feel like a shopping list that never ends.
With many traditional feeding setups, you’re layering product after product: a base mix, a balancer, added oil, digestive support, biotin, muscle support… the list goes on. Not only is this way of feeding complicated, but it’s also easy to overdo or miss key nutrients.
We do things differently.
Pure Feed is designed to deliver everything your horse needs in one bag, combining high-quality fibre, essential vitamins and minerals, oils, and functional ingredients to support digestion, condition, and overall health.
That’s 6+ nutritional products, working together in a balanced way. No guesswork, no over-supplementing, no complicated routines.
Just a simpler, more effective way to feed.

Feeding shouldn’t feel like a shopping list that never ends.
With many traditional feeding setups, you’re layering product after product: a base mix, a balancer, added oil, digestive support, biotin, muscle support… the list goes on. Not only is this way of feeding complicated, but it’s also easy to overdo or miss key nutrients.
We do things differently.
Pure Feed is designed to deliver everything your horse needs in one bag, combining high-quality fibre, essential vitamins and minerals, oils, and functional ingredients to support digestion, condition, and overall health.
That’s 6+ nutritional products, working together in a balanced way. No guesswork, no over-supplementing, no complicated routines.
Just a simpler, more effective way to feed.



